|
4–7 The point of onset of Long COVID is imprecisely defined and has been proposed to range from 3 to 12 weeks after infection. Persistent symptoms after COVID-19 illness have been called ‘Long COVID’. The degree of persistence of neuropsychiatric symptoms in the post-acute and chronic phases after infection, however, remained far from clear. 3 Studies assessing the prevalence of depression, anxiety and post-traumatic stress in acute COVID-19 suggested specific psychiatric morbidity. 1, 2 Analyses subsequently confirmed many neuropsychiatric manifestations of acute infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), with non-specific symptoms such as fatigue and headache, the most commonly studied and reported in the early literature. The literature on longer-term consequences is still maturing but indicates a particularly high prevalence of insomnia, fatigue, cognitive impairment and anxiety disorders in the first 6 months after infection.Įarly in the COVID-19 pandemic, neuropsychiatric symptoms were identified as a prominent feature of coronavirus outbreaks. Neuropsychiatric symptoms are common and persistent after recovery from COVID-19. 
There was little or no evidence of differential symptom prevalence based on hospitalization status, severity or follow-up duration. Between-study heterogeneity was high ( I 2 = 79.6–98.6%). Only two studies reported symptoms in control groups, both reporting higher frequencies in COVID-19 survivors versus controls. The most prevalent neuropsychiatric symptom was sleep disturbance, followed by fatigue, objective cognitive impairment, anxiety and post-traumatic stress. Study quality was most commonly moderate. The mean duration of follow-up after COVID-19 was 77 days (range 14–182 days). From 2844 unique titles, we included 51 studies ( n = 18 917 patients). Subgroup analyses were conducted for COVID-19 hospitalization, severity and duration of follow-up. 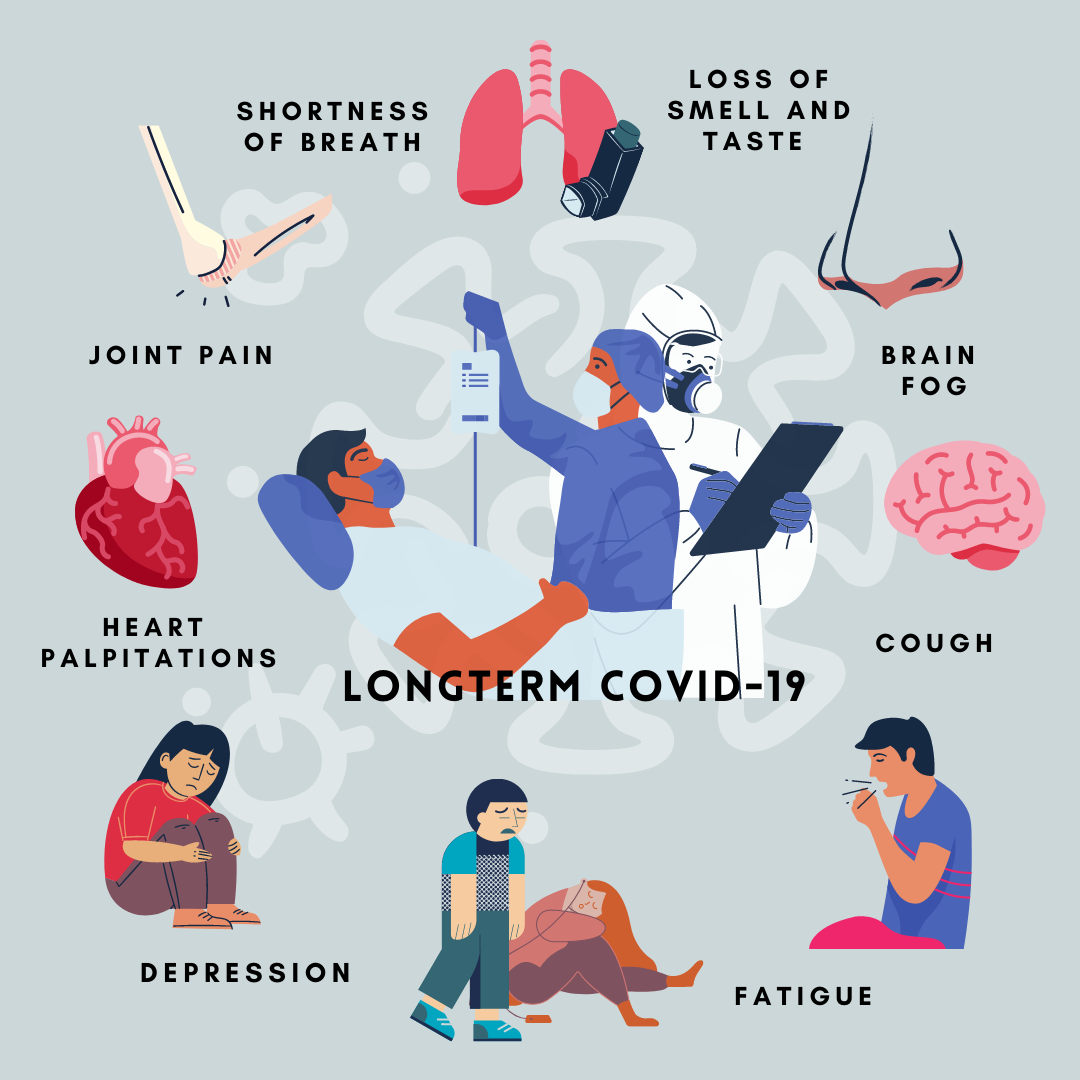
For each symptom, we calculated a pooled prevalence using generalized linear mixed models. For each study, a minimum of two authors extracted summary data. We included peer-reviewed studies reporting neuropsychiatric symptoms at post-acute or later time-points after COVID-19 infection and in control groups where available. For this pre-registered systematic review and meta-analysis (PROSPERO ID CRD42021239750), we searched MEDLINE, EMBASE, CINAHL and PsycINFO to 20 February 2021, plus our own curated database. To help inform mental health service planning in the pandemic recovery phase, we systematically determined the prevalence of neuropsychiatric symptoms in survivors of COVID-19. The nature and extent of persistent neuropsychiatric symptoms after COVID-19 are not established.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
